Antibodies Shown to Provide Long-term Immunity Against COVID-19
Using a highly accurate test they developed, University of Arizona Health Sciences researchers have shown that antibodies persist for months after infection.
When it comes to viruses, there are some similarities that are universal – but it’s the differences among viruses that make the diseases they cause notoriously difficult to treat. When a new virus such as SARS-CoV-2 appears, questions outweigh answers. How does the virus infect people? How does it spread? How contagious or deadly is it? And, most importantly, can it be stopped?
As COVID-19 became a global pandemic, scientists around the world worked relentlessly to answer those questions. At the University of Arizona Health Sciences, researchers in the College of Medicine – Tucson took an early interest in the novel coronavirus, which appeared to be affecting the elderly at a disproportionate rate.

Janko Nikolich-Žugich, MD, PhD, is internationally recognized as a leading immunologist and gerontologist.
Their eventual finding – that a highly accurate antibody test they developed shows immunity to COVID-19 is long-lasting – is poised to influence the way researchers and public health officials view the disease and seek to minimize its impact.
“My laboratory interest is to understand why older people get severely affected by infections. When the coronavirus epidemic broke out, it fit the bill perfectly for us,” said Janko Nikolich-Žugich, MD, PhD, head of the Department of Immunobiology and co-director of the Arizona Center on Aging. “We really needed to study the virus, but we had to have an antibody test to know who was exposed and who was not, and also as a means to begin to understand which parts of the virus our immune system is targeting to prevent the virus from doing harm.”
Dr. Nikolich-Žugich, whose research focuses on immunity and T cells, which function by directly killing infected host cells, reached out to Deepta Bhattacharya, PhD, an associate professor of immunobiology. Dr. Bhattacharya studies antibody-mediated immunity and B cells, which play a key role in antibody production. Both researchers are key contributors to Creating Defenses Against Disease, a UArizona Health Sciences’ strategic initiative designed to unravel the complexities of the immune system to enhance our ability to fight against disease.
As Dr. Bhattacharya’s research team developed viral assays specific to SARS-CoV-2 and neutralization assays to detect antibodies that can stop the virus, Dr. Nikolich-Žugich’s lab members carried out testing and validation. At the Center for Applied Genetics and Genomic Medicine, Ryan Sprissler, PhD, and his team analyzed the results and provided data-driven feedback.
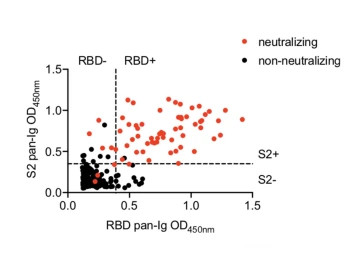
The high level of accuracy of the Health Sciences antibody test is shown by the lone black dot in the RBD+/S2+ region of this scatter plot. It represents the single false positive result that was identified during the study.
The work caught the attention of UArizona President Robert C. Robbins, MD, who tasked Health Sciences Senior Vice President Michael D. Dake, MD, with scaling the project from a departmental research endeavor to a statewide testing initiative fueled by a $3.5 million commitment from Gov. Doug Ducey.
“When we started, the first test we developed was 99% accurate for measuring antibodies in one part of the virus,” Dr. Nikolich-Žugich said. “We decided to confirm and hopefully improve that accuracy level by looking at another part of the virus that makes antibodies independently of the first location. We then validated that test, knowing some people will make antibodies more consistently for one part of the virus than the other. We put the two tests together, and only people who show antibody production for both parts of the test are determined to be positive.”
(left to right) Jennifer Uhrlaub and Rachel Wong perform assays in Dr. Nikolich-Žugich’s lab.
The scientific verification of the accuracy of the UArizona Health Sciences antibody test, which received U.S. Food and Drug Administration emergency use authorization, is highlighted in a paper recently published in Immunity. Out of 5,882 tests completed in Pima County – the first phase of the statewide testing initiative– only one returned a false positive, a rate of less than .02%
Drs. Nikolich-Žugich and Bhattacharya conducted follow-up testing on people who tested positive for antibodies. The results were clear: high-quality antibodies against SARS-CoV-2 persisted, providing long-term immunity against COVID-19.
“We clearly see high-quality antibodies still being produced five to seven months after SARS-CoV-2 infection,” said Dr. Bhattacharya. “Many concerns have been expressed about immunity against COVID-19 not lasting. We used this study to investigate that question, and we found that immunity is stable for at least five months.”
When a virus first infects cells, the immune system deploys short-lived plasma cells that produce antibodies to immediately fight the virus. Those antibodies appear in blood tests within 14 days of infection. The second stage of the immune response is the creation of long-lived plasma cells, which produce high-quality antibodies that provide lasting immunity.

In Pima County, 5,885 people were tested at multiple locations, such as the Pima County Health Department. The statewide initiative has the capacity to test 250,000.
Earlier studies extrapolated antibody production from initial infections and suggested antibody levels drop quickly after infection, providing only short-term immunity. Dr. Bhattacharya believes those extrapolations focused on short-lived plasma cells and didn’t take into account long-lived plasma cells and the high-affinity antibodies they produce.
“The latest time-points we tracked in infected individuals were past seven months, so that’s the longest period of time we can confirm immunity lasts,” Dr. Bhattacharya said. “That said, we know that people who were infected with the first SARS coronavirus, which is the most similar virus to SARS-CoV-2, are still seeing immunity 17 years after infection. If SARS-CoV-2 is anything like the first one, we expect antibodies to last at least two years, and it would be unlikely for anything much shorter than that.”
Dr. Nikolich-Žugich said the team now has tested almost 30,000 people in Arizona. Antibody tests are available for anyone in Arizona age 18 and older at locations around the state. Visit https://covid19antibodytesting.arizona.edu/ for more information and to sign up for testing.
Contact
Stacy Pigott
Office of Communications
520-539-4152
spigott@arizona.edu

